Improvements in Cancer Diagnoses
08 Sep 2015
New treatments, medicine and detection advancements are helping to slowly win the battle against this leading killer among men and women

By JESSICA SMITH
No matter what separates us from one another, human beings – unlike animals – share at least one commonality: the recognition of our imminent mortality. In the United States, cancer in all its forms is the second leading cause of death, exceeded only by heart disease. In 2015, the American Cancer Society estimates that there will be 1,658,370 new cancer diagnoses, as well as a sobering 589,430 cancer-related deaths.
Unlike days of old, however, a cancer diagnosis is no longer equivalent to an immediate death sentence. In fact, the mortality data shows that cancer death rates have decreased steadily over the last several years, by 1.8% per year for men and 1.4% per year for women. Here in Wilmington, cancer patients are fortunate to have access to a nationally acclaimed cancer center, with highly trained specialists and centralized support services designed to guide patients through the stages of care.
In 2001, New Hanover Regional Medical Center opened the Zimmer Cancer Center, southeastern North Carolina's only community cancer center dedicated solely to the diagnosis, treatment and support of cancer patients. The center houses outpatient services, including chemotherapy, infusion therapy and radiation therapies. Surgical procedures take place at the hospital’s Surgical Pavilion, opened in 2008. “The design of our cancer program is very good for patients,” says Dr. Cyrus Kotwall, surgical oncologist and medical director of the Zimmer Cancer Center. “They can see their radiation doctor, medical oncologist and surgeons at the same time, which helps tremendously with care coordination.”
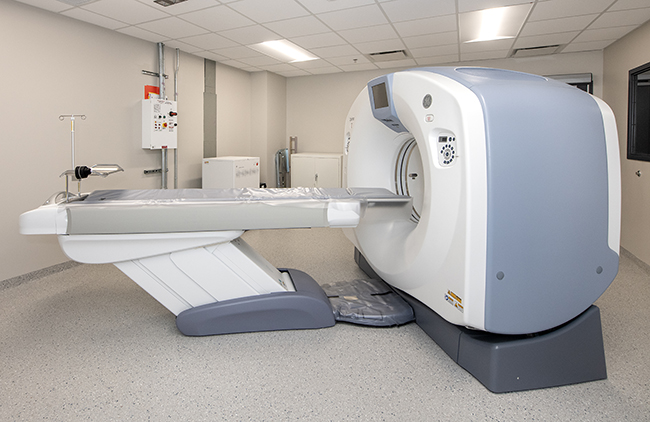
Many cancer patients are first diagnosed by their family physician, usually with a CT scan. After staging, or the process of determining the extent of cancer in the body, patients are referred to either a medical, radiation or surgical oncologists. Patients in an advanced stage, or those who have particularly complex cases, are referred to a multidisciplinary team of oncologists at a specialty facility. “Just a decade ago, patients who were diagnosed with difficult cases usually travelled to Duke or Chapel Hill for treatment,” says Dr. Kotwall. “As our program has grown and we’ve won more accolades for the way we practice, we’re experiencing a huge influx from all over the state, and even from South Carolina.”
Of the patients treated at the Zimmer Cancer Center, the largest percentage is afflicted with breast cancer, with lung cancer patients a close second. Patients with colon and rectal cancer, ovarian cancer and prostate cancer also represent a high volume of cases.
In addition to radiation and chemotherapy, many complex cases also require surgical oncology procedures to remove all or part of a cancerous growth. The majority of surgeries at the Center are conducted in the traditional open-body manner, but some specialties are able to take advantage of the facility’s state-of-the-art da Vinci Robotic Surgery system. The Center’s resident gynecological oncologists, Drs. Walter Gajewski and LucyBeth Nieves, perform many surgeries for ovarian cancer using this sophisticated robotic platform. By allowing surgeons to operate via a few small incisions in the patient’s body, the non-invasive system ultimately minimizes the patient’s pain, blood loss and scarring.
As the surgeon sits at a console, viewing a magnified, high-definition 3D image of the interior of the patient’s body, computer technologies scale and translate the surgeon’s hand movements into refined gesticulations of the instruments inside the patient’s body. “With robotic technology, the patient’s healing time is much faster. You can come in for surgery and go home the next day or the following day,” says Dr. Gajewski.
The team-based approach is a fundamental philosophy at the Center, which prefers a collaborative approach to the interpretation and analysis of complex cases. The team holds weekly “tumor boards” in which an array of medical, oncological, surgical, and diagnostic specialists convene to review the case files of a few patients at a time. They study all pathology and CAT scans, and together they devise the best possible treatment plan for each individual. “Our patients appreciate being discussed in the tumor boards,” says Dr. Kotwall. “When everyone agrees on the best approach — chemotherapy followed by surgery, or whatever the case may be — the patient benefits.”
Due to the immense need in our region, the Center’s primary goal is to increase the volume of patients it can accommodate. “Unfortunately, there is great demand,” says Dr. Kotwall. “We are also seeing an increase in our lung cancer cases, which makes sense considering the number of people who smoke here in the South. We’ve hired a new cardiovascular and thoracic surgeon, Dr. Kelly Nagasawa, to help treat these patients.” A new multidisciplinary clinic dedicated to the treatment of lung cancer is slated to open in the fall.
The Center also hosts an acclaimed clinical trials program, which gives patients a chance to participate in a wide array of trials, testing new chemotherapy drugs, as well as new radiation and surgical protocols.
“In a clinical trial, half of the patients may receive the standard chemotherapy drug, while the other half receives the new drug,” explains Dr. Kotwall. “Down the road, if the results prove that the new treatment is more effective, we’re able to participate in changing the standard of care for that particular type of cancer.”
One example of such a change is the breast cancer drug tamoxifen. While the drug was previously given only after chemotherapy, large-scale trials found that it was just as effective as chemotherapy when given alone. Current studies are examining the outcomes from prescribing tamoxifen as a preventative measure, to women who do not yet have breast cancer but who do have a family history.
In 2008, the cancer program at Zimmer was re-designated as a national Teaching Hospital Program by the American College of Surgeons’ Commission on Cancer, a prestigious accreditation received by only 25 percent of American cancer programs. “We work with medical students in their third or fourth year at UNC Chapel Hill,” says Dr. Kotwall. “We get residents in surgery, internal medicine, obstetrics and gynecology and family medicine, and we teach them everything we know about oncology.”
For a newly diagnosed cancer patient, the sheer volume of information can be overwhelming. Fortunately, the Wilmington area hosts a number of support organizations. “When you’re diagnosed, you tend to forget everything the doctors tell you. We provide journals to facilitate better communication with your medical team,” says Mary Barto, co-founder of She Rocks, Inc.
Established in 2014 upon Barto’s best friend Beth Quinn’s diagnosis with stage 4 ovarian cancer, the She Rocks foundation is a nonprofit fundraising and support organization (www.she-rocks.org). The group donates three-quarters of the funds it raises to UNC Lineberger Comprehensive Cancer Center in Chapel Hill, earmarked for the development of better diagnostic tools for ovarian cancer. The remainder of the money returns to our community to support local cancer patients.
“Along with bigger items like chemotherapy infusion chairs, we help with necessities like gas cards for commuting patients, and creature comforts, such as wigs and warm nightcaps for patients who’ve lost their hair, or Vitamin E cream to help with cracked skin,” says Barto. “When you have cancer, you need someone to reach in and support you, and sometimes friends and family have a hard time knowing what to say.”
Barto stresses that when it comes to your health, the most important thing to remember is to trust your instincts. “Pay attention to your own body, and listen to your symptoms,” she says. Early detection is critical, and excellent medical care and an extensive support network can make all the difference. In Wilmington, we're lucky enough to have both.
Understanding Prostate Cancer
Aside from skin cancer, more American men are diagnosed with prostate cancer than any other type. In fact, approximately one in seven men will be diagnosed with prostate cancer during his lifetime. Prostate cancer is also the second most common cause of cancer death, behind only lung cancer. The good news is that while prostate cancer can certainly be fatal if not detected in time, the vast majority of men with prostate cancer survive the disease.
Often described as the size of a large walnut, the prostate gland is part of the exocrine system, which secretes different types of fluids from and around the body via ducts. The salivary glands, sweat glands and mammary glands are also part of this system.
While men with advanced prostate cancer might suffer from incontinence, difficulty urinating or loss of bowel control, most men in the early stages of the disease have no discernible symptoms. Prostate cancer is a very slow-growing cancer, and new cases are generally found by screening patients at regular doctor’s appointments.
The risk of developing prostate cancer rises as men age, which is why medical opinion recommends routine screening as men enter their fifties. The most common screening test is known as the prostate-specific antigen (PSA) blood test, usually performed by your family physician. After a blood sample is taken from a vein in your arm, your blood is analyzed for abnormally high levels of a specific antigen, which may indicate prostate infection, inflammation or cancer.
The second most common screening test is the digital rectal exam (DRE). During a physical, your doctor examines your prostate via your rectum in order to determine if there are any abnormalities in the shape or size of the gland. Abnormalities on a DRE or PSA test usually lead either to a transrectal ultrasound, which uses sound waves to make a picture of your prostate gland, or a prostate biopsy, which uses a thin needle to collect tissue for analysis.
In the last three years, there has been considerable controversy over best practices in prostate cancer screening. Many organizations, including the U.S. Preventive Services Task Force and the Centers for Disease Control, no longer recommend routine screenings for prostate cancer using either the PSA or DRE. These organizations are concerned that excessive screening leads to over-diagnosis of prostate cancers, and is not evidence-based medicine.
Men are left without a definitive answer to the question: to screen or not to screen? The American Cancer Society’s recommendation is that men should make an informed decision after talking with their doctors about the risks and benefits of screening. The organization recommends that this conversation should occur between age 40 to 45 for men with the highest risk of developing prostate cancer, and age 50 for everyone else.
So what are the risk factors? Men with a family history of the disease — particularly those whose fathers and brothers have had prostate cancer — are more likely to contract it themselves, especially if the afflicted relative was diagnosed at a young age. In the United States, African-American men are more likely to get prostate cancer than men of other races. Obesity also seems to be a risk factor for prostate cancer, as does eating a diet heavy in red meat and high-fat dairy products.
Ironically enough, finding the disease long before symptoms occur may not improve your health in the long run. On the other hand, if you do have prostate cancer, it’s far better to discover it while the cancer is still confined to your prostate gland. Medical organizations do agree on one thing: the importance of talking to your doctor about your risk factors, your screening options and your overall health.
Preventing Skin Cancer
Whether or not we choose to follow current medical advice, most adults know that annual physicals, as well as biannual dentist visits, increase your chances of staying healthy. Far fewer of us realize that regular dermatological appointments should also be a priority.
The American Cancer Society recommends skin cancer-related checkups and sun exposure counseling beginning at age 20, for both genders. Dr. Rosalyn George, dermatologic surgeon at the Wilmington Dermatology Center, stresses that every individual should have annual skin checks – and if you have a history of skin cancers, that frequency should increase. One in five Americans will develop skin cancer in the course of a lifetime.
“Sun prevention is critical, especially for the young,” explains Dr. George. “If you have experienced five or more sunburns before the age of 18, your risk of developing melanoma actually doubles.” Dr. George recommends staying in the shade as much as possible, and wearing protective clothing, hats and sunglasses when you must be outside. She also insists upon sunscreen with a high SPF factor (30+) for daily use, no matter the season.
“Most people are good about applying sunscreen when they're at the beach or out on the water, but they forget about incidental exposure,” says Dr. George. “When you're shopping at Mayfaire or watching your kid's soccer game, that's the sun we don't count.”
Despite recent press about the efficacy of spray sunscreens, Dr. George maintains that they’re perfectly safe if used as directed. “It's not insect repellant. They are meant to be sprayed on your hand and rubbed into the skin.”
At Wilmington Dermatology Center, about half of new patients first come in when they notice a suspicious mole or spot. “We check every patient who walks in the door,” says Dr. George. “We've discovered plenty of skin cancers on patients who just came in for an acne or psoriasis treatment.”
So what should you be looking out for? There are three main categories of skin cancer. The most common, basal cell carcinoma, often presents as a shiny or pearly bump, or an open sore that fails to heal. The second most common skin cancer, squamous cell carcinoma, frequently looks like a reddish or brownish patch, often with a rough or scaly surface.
Both of these cancers can often be treated by chemotherapy creams and surgical removals, although some do require radiation. Many are removed with electrodessication and curettage, or the process of scraping away cancerous tissue before burning away any remaining cancerous cells with pulses of an electric current.
The most serious skin cancer, malignant melanoma, originates in melanocytes, also known as tanning cells. Voluntary tanning is thought to be one of the culprits for the recent rise in melanoma among young women, particularly those under 30. “This year, North Carolina banned the practice of using tanning beds for kids under age 18,” says Dr. George. “Hopefully, we’ll soon see the positive effects of that legislation.”
When a melanoma is discovered, surgical treatment options depend upon the depth of the melanoma as well as its location. Dr. George and her staff remove shallow melanomas in-house, excising an area of healthy skin around the periphery of the melanoma in order to be certain that all cancerous tissue is removed. If the melanoma is in a sensitive spot, such as on the nose or ear, the team uses Mohs micrographic surgery to preserve as much tissue as possible. For serious melanomas with a depth greater than 0.75 mm, the team refers the patient to a surgical oncologist. In these cases, the patient's lymph nodes are also checked, as the cancer may have spread to the lymph nodes or metastasized throughout the body.
If caught early, malignant melanoma is almost 100% curable, but it can be fatal if not treated promptly. Of the seven most common cancers in the US, melanoma is the only one in which cases are increasing, at a rate of almost 2 percent annually. “I cannot say it enough: please, get your skin checked once a year,” says Dr. George. “We can make a tremendous difference in our patients’ lives by detecting a skin cancer early on. But this only works if they walk in the door.”